Labral Repair & Shoulder Dislocation NJ
The Shoulder Center
at Modern Orthopedics of New Jersey
Paramus
72 Route 17 North
Paramus, NJ 07652
Wayne
2025 Hamburg Turnpike
STE C, Wayne, NJ 07470
Parsippany
3799 US-46
#207, Parsippany, NJ 07054
Shoulder Dislocation, Instability, and Labral Repair: Comprehensive Care for Joint Health
Understanding Shoulder Dislocation
Shoulder dislocation is a condition where the upper arm bone (humerus) is forced out of its natural position within the cup-shaped socket (glenoid) of the shoulder blade. A dislocated shoulder is not merely a result of the shoulder’s unique structure but a testament to its remarkable mobility – a feature that also makes it vulnerable to dislocation. Dislocation occurs when the head of the humerus partially or completely slips out of the circular glenoid, leading to instability and potential damage to supporting soft tissues and ligaments.
The human shoulder, with its incredible range of motion, is a highly mobile joint that plays a vital role in daily activities. However, its complexity means that an unexpected slip, fall, injury or collision can cause a dislocation, requiring immediate medical care. Severe pain often accompanies a dislocated shoulder, particularly after it has been put back into place.
Common Causes of Shoulder Dislocation:
-
Car accidents
-
Falls
-
Sports injuries, especially during contact sports like football, rugby, or lacrosse
-
Seizures (which can cause posterior dislocations)
Symptoms of a Dislocated Shoulder:
-
Severe shoulder pain
-
Visual deformity of the shoulder area
-
Swelling and bruising around the shoulder joint
-
Loss of range of motion
-
Muscle spasms
-
Numbness or tingling in the affected arm
If you experience these symptoms, seek professional help without delay.
Diagnosis and Treatment
Diagnosis often involves a visual inspection, medical history, and X-rays to confirm the dislocation and check for associated fractures. An MRI may be recommended to assess damage to other shoulder structures like the labrum, capsule, or rotator cuff.
Immediate treatment involves a reduction procedure to put the shoulder back in place. Following reduction, an orthopaedic evaluation will determine if other structures were injured and guide the treatment plan.
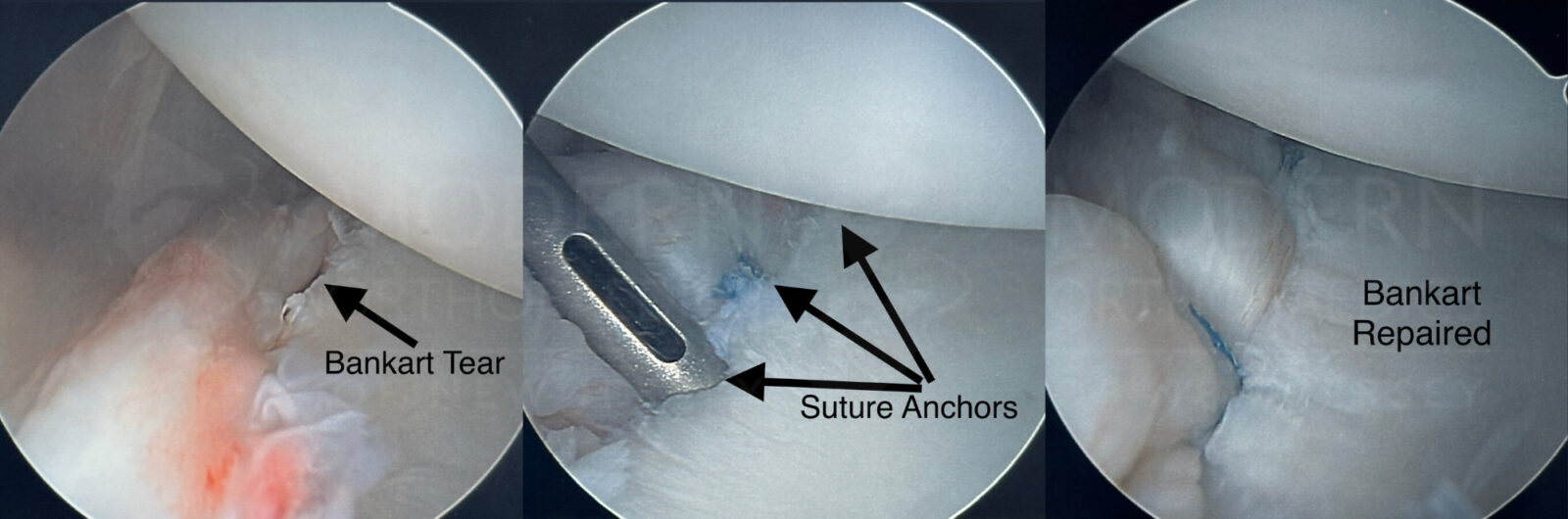
Arthroscopic Labral Repair: A Precise Approach to Healing
The labrum is a ring of cartilage surrounding the shoulder’s socket, providing stability and support. Damage to the labrum can lead to shoulder instability, pain, weakness, and further complications. Potential damage to the shoulder socket may also occur, requiring surgical intervention.
At our clinic, we specialize in arthroscopic labral repair, a minimally invasive surgical procedure aimed at restoring the labrum’s natural position. By utilizing specialized anchors and sutures, we secure the labrum in place, allowing the healing process to begin.
Postoperative Care: A Tailored Recovery Path
Recovery from arthroscopic labral repair is a carefully monitored journey. Within the first two weeks, we encourage gentle motion to prevent stiffness, always under professional guidance. Approximately several weeks to two months post-surgery, patients may progress to stretching and strengthening exercises as part of a tailored physical therapy plan.
Expect a full recovery from shoulder injury within three to six months, with our team supporting you every step of the way. We’re not just committed to the technical aspects of your healing, but to your overall well-being and a swift return to your daily routine.
Your Health, Our Priority
Shoulder dislocation and labral repair are complex but treatable conditions. Trust in our experience and patient-focused approach as we guide you through diagnosis, treatment, and recovery. Your health is our priority, and we’re here to ensure a smooth and successful healing process. Contact us today to learn more.


A Different Orthopedic Experience.
We combine cutting-edge technology with personalized care to deliver exceptional orthopedic treatment. Our team of experts focuses on your unique needs to ensure optimal outcomes and a superior healing experience.
Our Approach to Care
Comprehensive solutions for your orthopedic needs
Treatment Diversity
We offer a comprehensive range of treatments, ensuring personalized, targeted plans for every patient.
Technological Excellence
We utilize cutting-edge technology for precise diagnosis and innovative treatment options.
Collaborative Care
Our multi-disciplinary approach involves various specialties to provide comprehensive care and recovery.
Skilled Experts
Our team is composed of highly skilled, experienced orthopedic professionals, providing expert care.
Patient Focus
We prioritize patient comfort and satisfaction, creating a supportive environment for optimal healing.
Post-Treatment Support
Our robust post-treatment support ensures ongoing patient care through recovery and rehabilitation services.