Knee Doctors in New Jersey
The Modern
Knee Center of NJ
Here at Modern Orthopaedics of New Jersey, Dr. James Lee Jr. and Dr. Stern have advanced training and specialize specifically in non-surgical and surgical treatments on the knee.


ATo Knee Treatments
Knee Pain
At Modern Orthopedics, we understand that every shoulder is unique, just like the patients we serve. Your knees play an essential role in your daily life, from performing simple tasks to engaging in your favorite activities. That’s why we’re committed to providing individualized care that targets your specific needs.
Knee Exam & Diagnosis
Your journey to healing begins with a detailed diagnosis. Our skilled orthopedic specialists spend quality time understanding your symptoms, medical history, and lifestyle. Utilizing advanced diagnostic tools, we craft a comprehensive picture of your knee’s condition, ensuring an accurate diagnosis.
Tailored Knee Treatments
We believe that your treatment should be as unique as you are. After diagnosing your knee condition, our team collaborates with you to develop a treatment plan tailored to your individual needs and daily life. Whether it’s rehabilitation exercises, medication, or surgical intervention, our approach is focused on your well-being.
Your Partner In Pain-Free
We don’t just treat your shoulder; we partner with you in your recovery journey. Our dedicated team supports you every step of the way, providing continuous guidance and encouragement. We adapt our methods to align with your progress and preferences, ensuring a comfortable and effective recovery process.
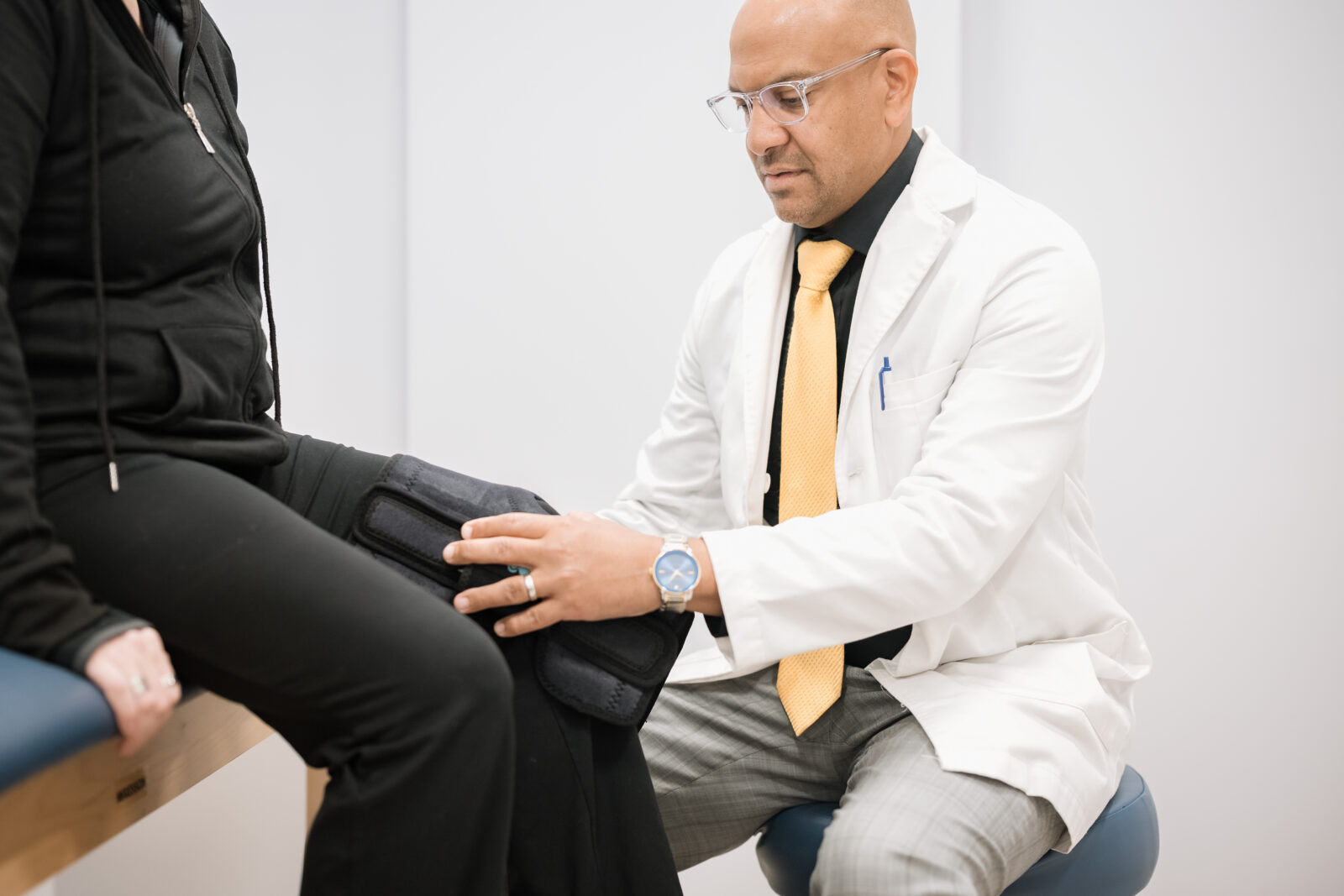
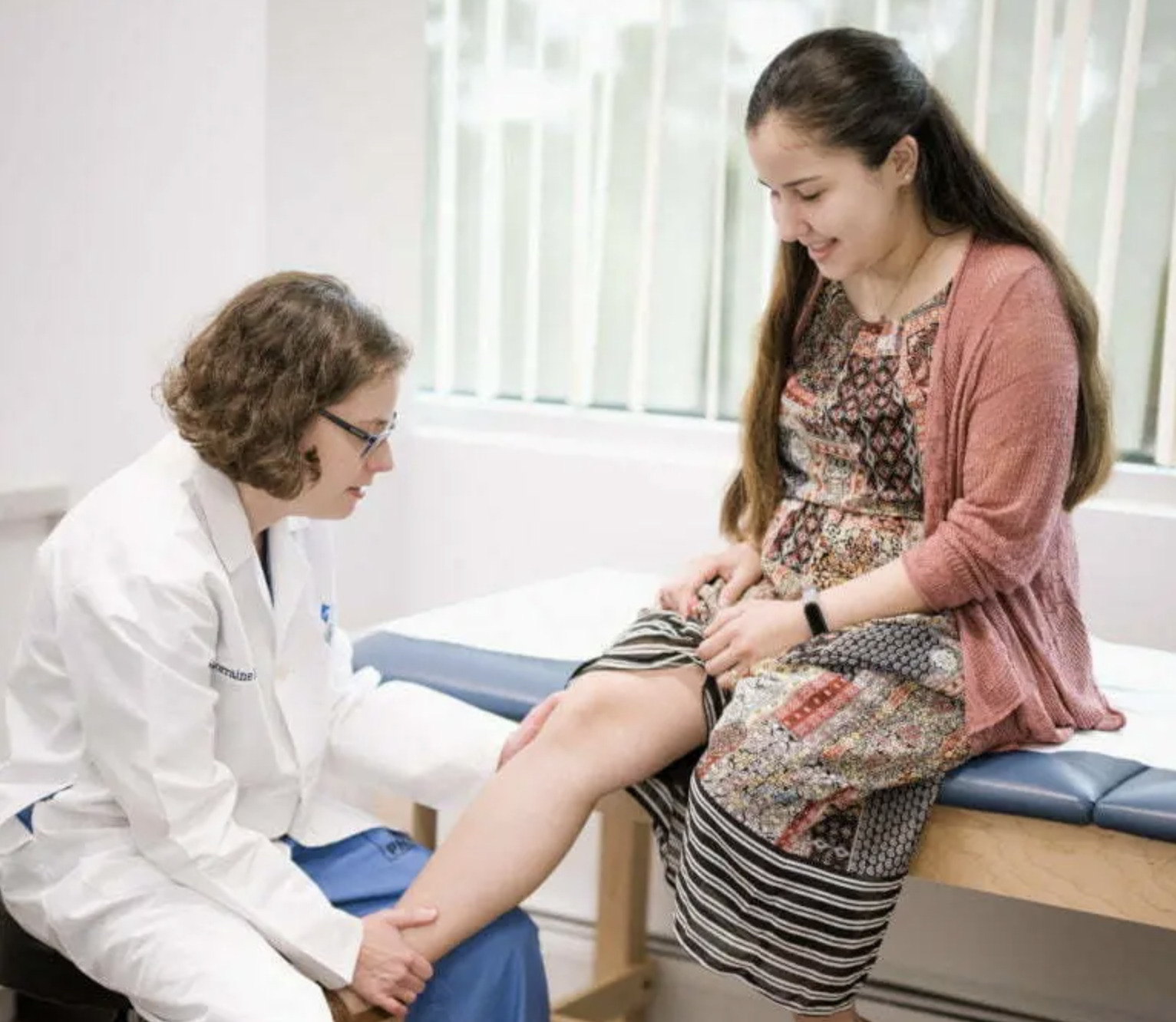
We specialize in a variety of
Conditions & Procedures
learn more below
Frequently Asked Questions about Knee Arthritis
What is knee arthritis?
Knee arthritis occurs when the cartilage covering of your knee joint wears down. The cartilage is there to protect the bone and allow for smooth and pain free motion. When the cartilage is no longer present, the rough surfaces of the exposed bones rub against one another causing pain.
What symptoms might I be experiencing if I have knee arthritis?
Patients with knee arthritis typically experience pain in the knee joint when standing, walking or going up and down the stairs. You may feel that your knee feels swollen or stiff and find it difficult to participate in activities you once were able to do with ease. Some patients also experience a feeling that their knee is going to “give out.” You may also experience that when you move your knee a grinding noise or feeling occurs.
What causes knee arthritis?
Arthritis can be caused by many different things including older age, family history, prior injury to the knee joint, prior knee surgery and obesity. Often times there is no underlying cause that can be identified.
Are there any treatments for knee arthritis that do not involve surgery?
- Lifestyle modifications such as weight loss if you are overweight and switching to lower impact activities can lower stress across your knee joint
- Physical therapy to work on range of motion, stretching and strengthening
- Using a cane in the opposite arm to offload some of the force that is being transmitted through your knee (e.g. if your right knee hurts, use the cane in your left hand and vice versa)
- Tylenol or anti-inflammatory medications such as Motrin or Advil for pain relief (always speak with your primary care doctor before starting any medications)
- A cortisone injection into the knee joint can be done in the office to relieve pain
- Viscosupplementation (“gel shot”) injections into the knee joint can be done in the office to relieve pain
Recognized as Top Knee Specialty Doctors in New Jersey
At Modern Orthopedics of New Jersey, our 5-Star concierge-trained staff was designed to guide each unique patient through questions, scheduling, insurance, and anything else needed to ensure the best possible experience for our patients.
Paramus
72 Route 17 North
Paramus, NJ 07652
Wayne
2025 Hamburg Turnpike
STE C, Wayne, NJ 07470
Parsippany
3799 US-46
#207, Parsippany, NJ 07054



